Is i10 a valid ICD 10 code?
I10 is a valid billable ICD-10 diagnosis code for Essential (primary) hypertension. It is found in the 2020 version of the ICD-10 Clinical Modification (CM) and can be used in all HIPAA-covered transactions from Oct 01, 2019 - Sep 30, 2020. Essential hypertension is high blood pressure that doesn't have a known secondary cause.
How many ICD 10 codes are there?
- ICD-10 codes were developed by the World Health Organization (WHO) External file_external .
- ICD-10-CM codes were developed and are maintained by CDC’s National Center for Health Statistics under authorization by the WHO.
- ICD-10-PCS codes External file_external were developed and are maintained by Centers for Medicare and Medicaid Services. ...
Where can one find ICD 10 diagnosis codes?
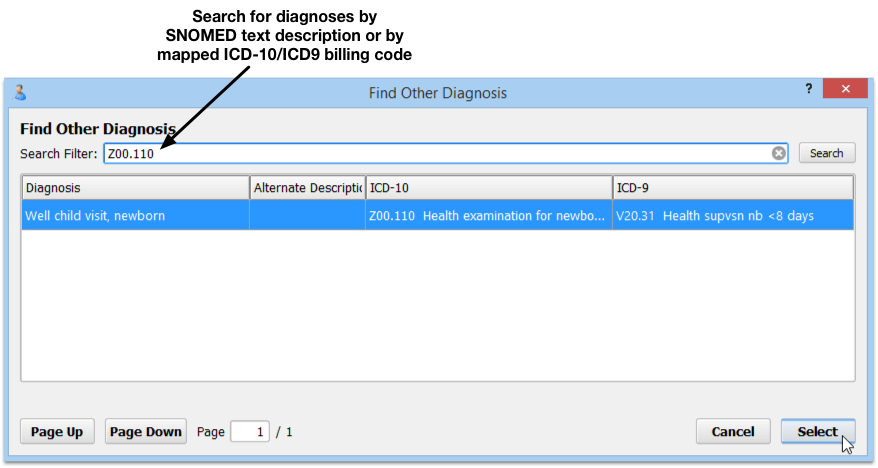
Search the full ICD-10 catalog by:
- Code
- Code Descriptions
- Clinical Terms or Synonyms
What are some examples of ICD codes?
ICD-9-CM codes are very different than ICD-10-CM/PCS code sets:
- There are nearly 19 times as many procedure codes in ICD-10-PCS than in ICD-9-CM volume 3
- There are nearly 5 times as many diagnosis codes in ICD-10-CM than in ICD-9-CM
- ICD-10 has alphanumeric categories instead of numeric ones
- The order of some chapters have changed, some titles have been renamed, and conditions have been grouped differently
What is the ICD-10 code for assistance with ADLS?
ICD-10-CM Code for Need for assistance with personal care Z74. 1.
What is the ICD-10 code for unable to care for yourself?
The 2022 edition of ICD-10-CM Z74. 1 became effective on October 1, 2021. This is the American ICD-10-CM version of Z74.
What is the ICD-10 code for nursing home placement?
Y92.12ICD-10 Code for Nursing home as the place of occurrence of the external cause- Y92. 12- Codify by AAPC.
What is the ICD-10 code for impaired mobility and ADLS?
Z74. 0 - Reduced mobility. ICD-10-CM.
What is the ICD-10 code for debility?
ICD-10 code R54 for Age-related physical debility is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
What is the ICD-10 code for functional decline?
VICC considers the correct code to assign for documentation of functional decline is R53 Malaise and fatigue following Index lead term Decline (general) (see also Debility) R53.
What is code Z51?
ICD-10 code Z51 for Encounter for other aftercare and medical care is a medical classification as listed by WHO under the range - Factors influencing health status and contact with health services .
What is the ICD-10 code for awaiting placement?
1 - Person awaiting admission to adequate facility elsewhere.
What is the CPT code for skilled nursing?
The annual nursing facility assessment is billed using CPT code 99318, and SNF discharge services are billed using CPT codes 99315-99316. Using an inpatient hospital E/M CPT code represents inappropriate billing when you render E/M services in an SNF.
What is the ICD-10 code for non ambulatory?
09: Other reduced mobility.
What is the ICD-10 code for decreased functional mobility?
Z74.0ICD-10-CM Code for Reduced mobility Z74. 0.
What is the ICD-10 code for mobility dysfunction?
ICD-10 code R26. 9 for Unspecified abnormalities of gait and mobility is a medical classification as listed by WHO under the range - Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified .
What is a Z00-Z99?
Categories Z00-Z99 are provided for occasions when circumstances other than a disease, injury or external cause classifiable to categories A00 -Y89 are recorded as 'diagnoses' or 'problems'. This can arise in two main ways:
Can you use Z59.0 for reimbursement?
Z59.0 should not be used for reimbursement purposes as there are multiple codes below it that contain a greater level of detail.
When will the Z74.2 ICd 10 be released?
The 2022 edition of ICD-10-CM Z74.2 became effective on October 1, 2021.
What is a Z00-Z99?
Categories Z00-Z99 are provided for occasions when circumstances other than a disease, injury or external cause classifiable to categories A00 -Y89 are recorded as 'diagnoses' or 'problems'. This can arise in two main ways:
What is the ICD code for home assistance?
Z74.2 is a billable ICD code used to specify a diagnosis of need for assistance at home and no other household member able to render care. A 'billable code' is detailed enough to be used to specify a medical diagnosis.
What is the approximate match between ICd9 and ICd10?
This is the official approximate match mapping between ICD9 and ICD10, as provided by the General Equivalency mapping crosswalk. This means that while there is no exact mapping between this ICD10 code Z74.2 and a single ICD9 code, V60.4 is an approximate match for comparison and conversion purposes.
What is billable code?
Billable codes are sufficient justification for admission to an acute care hospital when used a principal diagnosis.
When will the ICd 10 Z74.09 be released?
The 2022 edition of ICD-10-CM Z74.09 became effective on October 1, 2021.
What is a Z00-Z99?
Categories Z00-Z99 are provided for occasions when circumstances other than a disease, injury or external cause classifiable to categories A00 -Y89 are recorded as 'diagnoses' or 'problems'. This can arise in two main ways:
What are the requirements for Medicare homebound?
Medicare considers the beneficiary homebound if BOTH the following requirements are met: 1 the assistance of another person or the use of an assistive device – crutches, wheelchair, walker 2 It is difficult to leave home and he/she is unable to do so
What does "homebound" mean in medical records?
Documentation of homebound status "fits" entire medical record. All homebound documentation on the Plan of Care (POC) must be supported by documentation in the medical record. If the POC shows "endurance" is the reason the beneficiary is homebound, the documentation in the certifying physician's medical records and/or the acute/post-acute care facility's medical records should state why or how the limited endurance makes the beneficiary homebound.
What is home health agency?
The home health agencies documentation, such as the initial and/or comprehensive assessment of the patient can be incorporated into the certifying physician's medical record and used to support the patient's homebound status and need for skilled care.
How often should homebound status be documented?
The home health agency should document the homebound status frequently enough to reflect the beneficiary's current functional status, and at a minimum, at least once per episode. It is recommended that homebound status be documented in clear, specific, and measurable terms.
What documentation is needed to be certified for home health?
Documentation from the certifying physician's medical records and/or the acute/post-acute care facility's medical records is used to support the certification of home health eligibility. This documentation must support the patient's need for skilled services and homebound status.
When did the new definition of home health go into effect?
The new definition, which went into effect November 19, 2013, will prevent confusion, promote a clearer enforcement of the statute, and provide more definitive guidance to home health agencies in order to foster compliance, CMS says.
How far can a beneficiary walk before being short of breath?
Example: The beneficiary can only walk 10 feet before becoming extremely short of breath and diaphoretic at which time the beneficiary needs to rest. In addition, the beneficiary needs to hang onto furniture while walking. Simply documenting the use of a cane or walker in the POC does not reflect the homebound status.

Popular Posts:
- 1. icd 10 code for work conditioning
- 2. what is the icd 2019 10 code for myasthenia gravis in crisis
- 3. icd 10 code for adverse effect of namenda
- 4. icd 10 code for paroxysmal afib
- 5. icd 9 code for status post left bicep tendon repair
- 6. icd 10 code for follow up healed non-pressure ulcer
- 7. icd-10-pcs code for control of epistaxis
- 8. icd 10 code for swimmer's ear in the left ear
- 9. icd 10 cm code for abscess of the tonsil
- 10. icd 10 code for pleuritic chest pain