What is the ICD 10 code for nephropathy with diffuse membranous glomrlneph?
N07.2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. Short description: Hereditary nephropathy, NEC w diffuse membranous glomrlneph. The 2020 edition of ICD-10-CM N07.2 became effective on October 1, 2019.
What is the ICD 10 code for nephropathy?
N14.1 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. Short description: Nephropathy induced by oth drug/meds/biol subst. The 2020 edition of ICD-10-CM N14.1 became effective on October 1, 2019.
What is the ICD 10 code for Neurologic diagnosis?
N04.2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM N04.2 became effective on October 1, 2021. This is the American ICD-10-CM version of N04.2 - other international versions of ICD-10 N04.2 may differ.
What is the ICD 10 code for kidney failure?
N04.2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM N04.2 became effective on October 1, 2020. This is the American ICD-10-CM version of N04.2 - other international versions of ICD-10 N04.2 may differ. any associated kidney failure ( N17-N19 ).
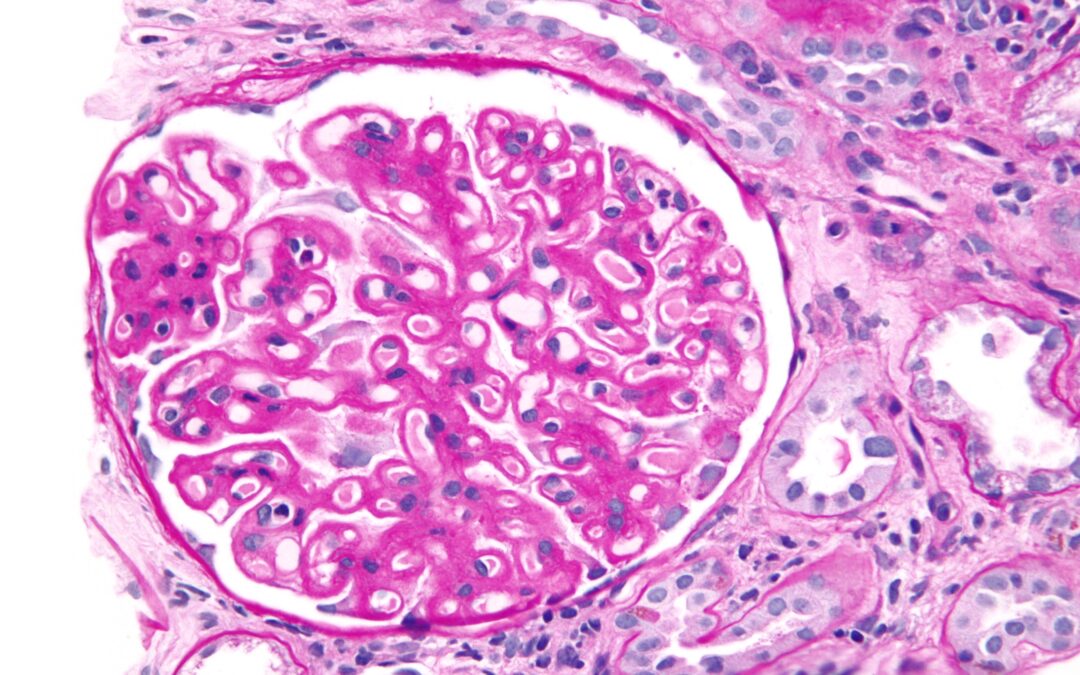
What is the ICD 10 code for membranous nephropathy?
ICD-10-CM Code for Nephrotic syndrome with diffuse membranous glomerulonephritis N04. 2.
What is membranous nephropathy?
Membranous nephropathy (MEM-bruh-nus nuh-FROP-uh-thee) occurs when the small blood vessels in the kidney (glomeruli), which filter wastes from the blood, become damaged and thickened. As a result, proteins leak from the damaged blood vessels into the urine (proteinuria).
Is nephrotic syndrome the same as membranous nephropathy?
The kidneys have filters that are responsible for cleaning waste products from your blood. In membranous nephropathy (MN), these filters are attacked by the body's immune system. Grouped together, the symptoms of this disease are called nephrotic syndrome.
Is membranous nephropathy the same as membranous glomerulonephritis?
Membranous glomerulonephritis (MGN) is a specific type of GN. MGN develops when inflammation of your kidney structures causes problems with the functioning of your kidney. MGN is known by other names, including extramembranous glomerulonephritis, membranous nephropathy, and nephritis.
Is membranous nephropathy a kidney disease?
Membranous Nephropathy (MN) is a kidney disease that affects the filters (glomeruli) of the kidney and can cause protein in the urine, as well as decreased kidney function and swelling. It can sometimes be called membranous glomerulopathy as well (these terms can be used interchangeably and mean the same thing).
What is the difference between nephritis and nephropathy?
Nephritis is inflammation of the kidneys and may involve the glomeruli, tubules, or interstitial tissue surrounding the glomeruli and tubules. It is one of several different types of nephropathy.
How is membranous nephropathy diagnosed?
A kidney biopsy is usually needed to confirm the diagnosis. It can tell your doctor the type of kidney disease you have, the amount of kidney damage and what treatments may work best. Anti-PLA2R antibody test. This new blood test looks for certain immune substances related to membranous nephropathy.
Is IgA nephropathy nephrotic or nephritic?
IgA nephropathy is a nephritic syndrome, a form of chronic glomerulonephritis. Often... read more characterized by the deposition of IgA immune complexes in glomeruli. It is the most common form of glomerulonephritis worldwide.
What does PLA2R mean?
PLA2R = M-type phospholipase A2 receptor, PMN = primary membranous nephropathy. In this study, among 136 patients, 5 patients had IgG4 but no PLA2R deposition. In this situation, a possible explanation for the result is that there could be another antigenic target of autoantibody driving the disease.
What is the ICD 10 code for glomerulonephritis?
Unspecified nephritic syndrome with diffuse membranous glomerulonephritis. N05. 2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM N05.
Is membranous glomerulonephritis primary or secondary?
Membranous nephropathy (MN) is a common cause of proteinuria and nephrotic syndrome all over the world. It can be subdivided into primary and secondary forms. Primary form is an autoimmune disease clinically characterized by nephrotic syndrome and slow progression. It accounts for ~70% cases of MN.
Is nephrotic syndrome a type of glomerulonephritis?
Glomerulonephritis is a group of diseases that injure the part of the kidney that filters blood (called glomeruli). Other terms you may hear used are nephritis and nephrotic syndrome.
What is the treatment for membranous nephropathy?
There is no specific treatment for membranous nephropathy. Supportive care with the use of diuretics and angiotensin-converting enzyme inhibitors in combination with angiotensin II receptor blocker is recommended, but these agents have only a limited effect.
Can membranous nephropathy be reversed?
There is no certain cure. However, up to three out of 10 people with membranous nephropathy have their symptoms completely disappear (remission) after five years without any treatment. About 25 to 40 percent have a partial remission.
Can you live a long life with proteinuria?
For example, the life expectancies of 40-year-old men and women with no proteinuria were 15.2 and 17.4 years longer, respectively, than those with heavy proteinuria. Proteinuria-free men and women also outlived those with mild proteinuria by 8.2 years and 10.5 years, respectively.
Popular Posts:
- 1. icd 10 code for non radiographic axial spondyloarthritis
- 2. icd-10 code for paranoid delusions
- 3. icd 10 code for first degree atrioventricular block
- 4. icd 10 code for respiratory failure on ventilator
- 5. what is the icd 10 code for nstemi
- 6. icd 10 code for sinus headache
- 7. 2018 icd 10 code for resection left calcaneal fracture
- 8. icd 10 code for cotton wool spot
- 9. icd-10 code for second degree av block
- 10. icd 10 cm code for bleeding mole on back