What is the ICD 10 code for venous insufficiency?
Oct 01, 2021 · Varicose veins of bilateral lower extremities with pain. 2016 2017 2018 2019 2020 2021 2022 Billable/Specific Code Adult Dx (15-124 years) I83.813 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM I83.813 became effective on October 1, 2021.
What is the ICD 10 code for varicose veins?
Oct 01, 2021 · Venous insufficiency (chronic) (peripheral) 2016 2017 2018 2019 2020 2021 2022 Billable/Specific Code. I87.2 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM I87.2 became effective on October 1, 2021.
What is the ICD 10 for stasis ulcer without varicose veins?
Dec 27, 2020 · Group 1 Medical Necessity ICD-10-CM Codes Asterisk Explanation *The venous malformations ICD-10-CM diagnosis code (Q27.8, other specified congenital malformations of peripheral vascular system) only applies to the foam sclerotherapy CPT codes 36465, 36466, 36470, and 36471.
What is the ICD 10 code for venous ulcer?
Billable codes are sufficient justification for admission to an acute care hospital when used a principal diagnosis. | ICD-10 from 2011 - 2016. I87.2 is a billable ICD code used to specify a diagnosis of venous insufficiency (chronic) (peripheral).
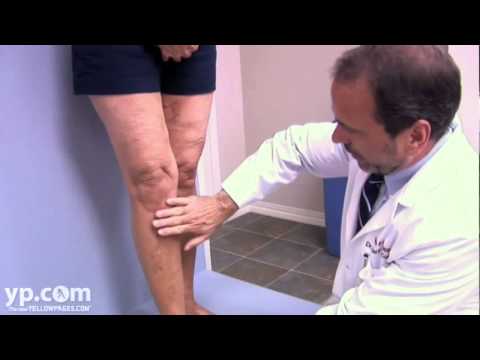
Is venous insufficiency the same as varicose veins?
What is Venous Insufficiency (Varicose Veins)? Venous insufficiency is a medical condition in which veins in the body (most often in the legs) are not able to pump blood back to the heart. This causes blood to pool in the blood vessels so that they become enlarged (varicose) or dilated over time.
What is the ICD-10 code for chronic venous insufficiency?
ICD-10 code: I87. 2 Venous insufficiency (chronic)(peripheral) - gesund.bund.de.
How do you code chronic venous insufficiency?
ICD-10 | Venous insufficiency (chronic) (peripheral) (I87. 2)
What is the diagnosis code for varicose veins?
Group 1CodeDescriptionI83.811Varicose veins of right lower extremity with painI83.812Varicose veins of left lower extremity with painI83.813Varicose veins of bilateral lower extremities with painI83.891Varicose veins of right lower extremity with other complications41 more rows
What is the ICD-10 code for PVD?
ICD-10 | Peripheral vascular disease, unspecified (I73. 9)
What is venous insufficiency chronic peripheral?
Chronic venous insufficiency (CVI) is a condition that occurs when the venous wall and/or valves in the leg veins are not working effectively, making it difficult for blood to return to the heart from the legs. CVI causes blood to “pool” or collect in these veins, and this pooling is called stasis. Valve Inside Vein.May 14, 2019
What is the correct ICD-10 code for thrombocytopenia?
ICD-10 | Thrombocytopenia, unspecified (D69. 6)
What is the CPT code 36475?
CPT® 36475, Under Endovascular Ablation Therapy of Incompetent Extremity Veins. The Current Procedural Terminology (CPT®) code 36475 as maintained by American Medical Association, is a medical procedural code under the range - Endovascular Ablation Therapy of Incompetent Extremity Veins.
What is ICD-10 code for osteoporosis?
ICD-9-CM and ICD-10-CM CodesOsteoporosis ICD-9-CM & ICD-10-CM CodesOSTEOPOROSISOsteoporosis unspecified: 733.00M81.0Senile osteoporosis: 733.01M81.0Idiopathic osteoporosis: 733.02M81.812 more rows
What is the CPT code 36471?
CPT® 36471, Under Sclerotherapy of Telangiectasia and Incompetent Veins. The Current Procedural Terminology (CPT®) code 36471 as maintained by American Medical Association, is a medical procedural code under the range - Sclerotherapy of Telangiectasia and Incompetent Veins.
What is the ICD-10 code for hyperlipidemia?
E78.5ICD-10 | Hyperlipidemia, unspecified (E78. 5)
Does Medicare cover 36471?
Compression Sclerotherapy (CPT codes 36470 and 36471) Medicare does not have a National Coverage Determination (NCD) for compression sclerotherapy. Local Coverage Determinations (LCDs)/Local Coverage Articles (LCAs) exist for all states/territories and compliance with these policies is required where applicable.Sep 21, 2021
General Information
CPT codes, descriptions and other data only are copyright 2020 American Medical Association. All Rights Reserved. Applicable FARS/HHSARS apply.
CMS National Coverage Policy
Title XVIII of the Social Security Act, Section 1833 (e) states that no payment shall be made to any provider of services or other person under this part unless there has been furnished such information as may be necessary in order to determine the amounts due such provider or other person under this part for the period with respect to which the amounts are being paid or for any prior period..
Article Guidance
This Billing and Coding Article provides billing and coding guidance for Local Coverage Determination (LCD) L38720 Treatment of Chronic Venous Insufficiency of the Lower Extremities.
ICD-10-CM Codes that Support Medical Necessity
It is the provider’s responsibility to select codes carried out to the highest level of specificity and selected from the ICD-10-CM code book appropriate to the year in which the service is rendered for the claim (s) submitted.
ICD-10-CM Codes that DO NOT Support Medical Necessity
All those not listed under the “ICD-10 Codes that Support Medical Necessity” section of this article.
Bill Type Codes
Contractors may specify Bill Types to help providers identify those Bill Types typically used to report this service. Absence of a Bill Type does not guarantee that the article does not apply to that Bill Type.
Revenue Codes
Contractors may specify Revenue Codes to help providers identify those Revenue Codes typically used to report this service. In most instances Revenue Codes are purely advisory. Unless specified in the article, services reported under other Revenue Codes are equally subject to this coverage determination.
What is the ICD code for venous insufficiency?
The ICD code I872 is used to code Chronic venous insufficiency. Chronic venous insufficiency (CVI) is a medical condition in which the veins cannot pump enough blood back to the heart. The most common cause of CVI is superficial venous reflux which is a treatable condition.
What is the ICD10 code for 459.81?
This means that while there is no exact mapping between this ICD10 code I87.2 and a single ICD9 code, 459.81 is an approximate match for comparison and conversion purposes.
What is CVI in legs?
As functional venous valves are required to provide for efficient blood return from the lower extremities, this condition typically affects the legs. If the impaired vein function causes significant symptoms, such as swelling and ulcer formation, it is referred to as chronic venous disease. CVI includes varicose veins and superficial venous reflux ...
What is the venous system?
The venous system of the lower extremities consists of the superficial veins (this includes the great and small saphenous and accessory, or duplicate, veins that travel in parallel with the great and small saphenous veins), the deep system (popliteal and femoral veins), and perforator veins that cross through the fascia and connect the deep and superficial systems. One-way valves are present within all veins to direct the return of blood up the lower limb. Because the venous pressure in the deep system is generally greater than that of the superficial system, valve incompetence at any level may lead to backflow (venous reflux) with pooling of blood in superficial veins. Varicose veins with visible varicosities may be the only sign of venous reflux, although itching, heaviness, tension, and pain may also occur. Chronic venous insufficiency secondary to venous reflux can lead to thrombophlebitis, leg ulcerations, and hemorrhage. The CEAP classification of venous disease considers the clinical, etiologic, anatomic, and pathologic characteristics of venous insufficiency, ranging from class 0 (no visible sign of disease) to class 6 (active ulceration).
What is the treatment for a great vein?
Treatment of the great or small saphenous veins by surgery (ligation and stripping), endovenous thermal ablation (radiofrequency or laser), microfoam sclerotherapy or cyanoacrylate adhesive may be considered MEDICALLY NECESSARY for symptomatic varicose veins/venous insufficiency when the following criteria have been met:
What is sclerotherapy in veins?
The objective of sclerotherapy is to destroy the endothelium of the target vessel by injecting an irritant solution (either a detergent, osmotic solution, or chemical irritant), ultimately occluding the vessel. Treatment success depends on accurate injection of the vessel, an adequate injectate volume and concentration of sclerosant, and compression. Historically, larger veins and very tortuous veins were not considered good candidates for sclerotherapy due to technical limitations. Technical improvements in sclerotherapy have included the routine use of Duplex ultrasound to target refluxing vessels, luminal compression of the vein with anesthetics, and a foam/sclerosant injectate in place of liquid sclerosant. Foam sclerosants are produced by forcibly mixing a gas (eg, air or carbon dioxide) with a liquid sclerosant (eg, polidocanol or sodium tetradecyl sulfate). Physician-compounded foam is produced at the time of treatment. A commercially available microfoam sclerosant with a proprietary gas mix is available that is proposed to provide smaller and more consistent bubble size than what is produced with physician-compounded sclerosant foam.
What veins travel in parallel with the great or small saphenous veins?
Saphenous veins include the great and small saphenous and accessory saphenous veins that travel in parallel with the great or small saphenous veins. Tributaries are veins that empty into a larger vein. Treatment of venous reflux has traditionally included the following:
Is a perforator vein ligation necessary?
Surgical ligation (including subfascial endoscopic perforator surgery) or endovenous radiofrequency or laser ablation of incompetent perforator veins may be considered MEDICALLY NECESSARY as a treatment of leg ulcers associated with chronic venous insufficiency when the following conditions have been met:
Can perforator veins be ablated?
For individuals who have perforator vein reflux who receive ablation (eg, subfascial endoscopic perforator surgery) of perforator veins, the evidence includes RCTs and systematic reviews of RCTs. Relevant outcomes are symptoms, change in disease status, morbid events, quality of life, and treatment-related morbidity. The literature has indicated that the routine ligation or ablation of incompetent perforator veins is not necessary for the treatment of varicose veins/venous insufficiency at the time of superficial vein procedures. However, when combined superficial vein procedures and compression therapy have failed to improve symptoms (ie, ulcers), treatment of perforator vein reflux may be as beneficial as an alternative (eg, deep vein valve replacement). Comparative studies are needed to determine the most effective method of ligating or ablating incompetent perforator veins. Subfascial endoscopic perforator surgery is possibly as effective as the Linton procedure with a reduction in adverse events. Endovenous ablation with specialized laser or radiofrequency probes has been shown to effectively ablate incompetent perforator veins with a potential decrease in morbidity compared with surgical interventions. The evidence is sufficient to determine that the technology results in an improvement in the net health outcome.
The ICD code I832 is used to code Venous ulcer
Venous ulcers (venous insufficiency ulceration, stasis ulcers, stasis dermatitis, varicose ulcers, or ulcus cruris) are wounds that are thought to occur due to improper functioning of venous valves, usually of the legs (hence leg ulcers).:846 They are the major occurrence of chronic wounds, occurring in 70% to 90% of leg ulcer cases.
ICD-10-CM Alphabetical Index References for 'I83.20 - Varicose veins of unspecified lower extremity with both ulcer and inflammation'
The ICD-10-CM Alphabetical Index links the below-listed medical terms to the ICD code I83.20. Click on any term below to browse the alphabetical index.
What is the venous system?
The venous system of the lower extremities consists of the superficial veins (this includes the greater and lesser saphenous, and accessory or duplicate veins that travel in parallel with the greater and lesser saphenous veins), the deep system (popliteal and femoral veins), and perforator veins that cross through the fascia and connect the deep and superficial systems. One-way valves are present within all veins to direct the return of blood up the lower limb. Since venous pressure in the deep system is generally greater than that of the superficial system, valve incompetence at any level may lead to backflow (venous reflux) with pooling of blood in superficial veins. Varicose veins with visible varicosities may be the only sign of venous reflux, although itching, heaviness, tension, and pain may also occur. Chronic venous insufficiency secondary to venous reflux can lead to thrombophlebitis, leg ulcerations and hemorrhage. The CEAP classification considers the clinical, etiologic, anatomic, and pathologic characteristics of venous insufficiency, ranging from class 0 (no visible sign of disease) to class 6 (active ulceration).
What are the saphenous veins?
Saphenous veins include the greater and lesser saphenous, and accessory saphenous veins that travel in parallel with the greater or lesser saphenous veins. Tributaries are veins that empty into a larger vein. Treatment of venous reflux typically includes the following:
What is the CPT code for stab phlebectomy?
There is no specific CPT code for transilluminated powered phlebectomy. Providers might elect to use CPT codes describing stab phlebectomy (37765 or 37766) or unlisted vascular surgery procedure (37799).
What is BCBSVT medical policy?
Blue Cross and Blue Shield of Vermont (BCBSVT) Medical Policies are developed to provide clinical guidance and are based on research of current medical literature and review of common medical practices in the treatment and diagnosis of disease. The applicable group/individual contract and member certificate language determines benefits that are in effect at the time of service. Since medical practices and knowledge are constantly evolving, BCBSVT reserves the right to review and revise its medical policies periodically. To the extent that there may be any conflict between medical policy and contract language, the member’s contract language takes precedence.
What is sclerotherapy in veins?
The objective of sclerotherapy is to destroy the endothelium of the target vessel by injecting an irritant solution (either a detergent, osmotic solution, or chemical irritant), ultimately resulting in the occlusion of the vessel. The success of the treatment depends on accurate injection of the vessel, an adequate injectate volume and concentration of sclerosant, and compression. Historically, larger veins and very tortuous veins were not considered to be good candidates for sclerotherapy due to technical limitations. Technical improvements in sclerotherapy have included the routine use of Duplex ultrasound to target refluxing vessels, luminal compression of the vein with anesthetics, and a foam/sclerosant injectate in place of liquid sclerosant. Foam sclerosants are produced by forcibly mixing a gas (e.g., air or carbon dioxide) with a liquid sclerosant (e.g., polidocanol or sodium tetradecyl sulfate). The foam is produced at the time of treatment and is considered an off-label use. A proprietary microfoam sclerosant (Varisolve, BTG PLC, London) with a controlled density and more consistent bubble sizes is being developed in Europe.
What is the procedure to open perforator veins?
Incompetent perforating veins were originally addressed with an open surgical procedure, called the Linton procedure, which involved a long medial calf incision to expose all posterior, medial, and paramedial perforators. While this procedure was associated with healing of ulcers, it was largely abandoned due to a high incidence of wound complications. The Linton procedure was subsequently modified by using a series of perpendicular skin flaps instead of a longitudinal skin flap to provide access to incompetent perforator veins in the lower part of the leg. The modified Linton procedure may be occasionally utilized for the closure of incompetent perforator veins that cannot be reached by less invasive procedures. Subfascial endoscopic perforator surgery (SEPS) is a less-invasive surgical procedure for treatment of incompetent perforators and has been reported since the mid-1980s. Guided by Duplex ultrasound scanning, small incisions are made in the skin and the perforating veins are clipped or divided by endoscopic scissors. The operation can be performed as an outpatient procedure. Endovenous ablation of incompetent perforator veins with sclerotherapy and radiofrequency has also been reported.
What is the ICD-10 code for varicose veins?
I83.10 is a billable diagnosis code used to specify a medical diagnosis of varicose veins of unspecified lower extremity with inflammation. The code I83.10 is valid during the fiscal year 2021 from October 01, 2020 through September 30, 2021 for the submission of HIPAA-covered transactions.#N#The ICD-10-CM code I83.10 might also be used to specify conditions or terms like dilated subcutaneous veins, dilated subcutaneous veins, extensive lipodermatosclerosis, fat necrosis of subcutaneous tissue, lipodermatosclerosis , lipodermatosclerosis of lower limb due to varicose veins of lower limb, etc.#N#The code I83.10 is applicable to adult patients aged 15 through 124 years inclusive. It is clinically and virtually impossible to use this code on a patient outside the stated age range.#N#Unspecified diagnosis codes like I83.10 are acceptable when clinical information is unknown or not available about a particular condition. Although a more specific code is preferable, unspecified codes should be used when such codes most accurately reflect what is known about a patient's condition. Specific diagnosis codes should not be used if not supported by the patient's medical record.
Where do varicose veins form?
Varicose veins are swollen, twisted veins that you can see just under the skin. They usually occur in the legs, but also can form in other parts of the body. Hemorrhoids are a type of varicose vein.
When to use I83.10?
Unspecified diagnosis codes like I83.10 are acceptable when clinical information is unknown or not available about a particular condition. Although a more specific code is preferable, unspecified codes should be used when such codes most accurately reflect what is known about a patient's condition.
Can you get varicose veins while pregnant?
You are more at risk if you are older, are female, have obesity, don't exercise, or have a family history of varicose veins. They can also be more common in pregnancy.

Popular Posts:
- 1. what is the icd 10 code for lesion in the base of tongue with hemorrhage
- 2. icd 9 code for aftercare pubic ramus fracture
- 3. icd 10 code for kyphoplasty present
- 4. icd 10 code for bitten by a vampire
- 5. icd 10 code for r18.8
- 6. icd 10 code for mild shortness of breath
- 7. icd 10 code for urithriis
- 8. icd 10 code for essential tremors of right hand
- 9. what icd 10 code to assign for a patient that comes for acucheck training
- 10. icd 10 code for junctional tachycardia