What is the ICD-O code for osteochondroma?
ICD coding ICD-O: 9210/0 - Osteochondroma ICD-11: 2E83.Y & XH5Y87 - Other specified benign osteogenic tumors and osteochondroma
What is the ICD 10 code for osteochondrosis of the humerus?
Osteochondrosis (juvenile) of capitulum of humerus [Panner]; Osteochondrosis (juvenile) of head of humerus [Haas] ICD-10-CM Diagnosis Code M92.1 Juvenile osteochondrosis of radius and ulna Osteochondrosis (juvenile) of lower ulna [Burns]; Osteochondrosis (juvenile) of radial head [Brailsford]
What are the different forms of osteochondromas?
Osteochondromas can develop as a single tumor (osteocartilaginous exostosis) or as many tumors (multiple osteochondromatosis). Because symptoms and treatment options may vary depending on which form a patient has, this article discusses them separately.
How do you test for osteochondroma?
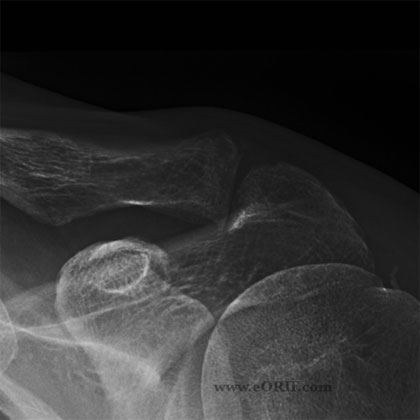
In order to diagnose osteochondroma, your doctor will order imaging tests. X-rays. These tests provide clear pictures of dense structures like bone, and will show the bony growth of an osteochondroma. Other imaging scans.
What is the ICD-10 code for osteochondroma?
D16.9Benign neoplasm of bone and articular cartilage, unspecified D16. 9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM D16. 9 became effective on October 1, 2021.
How do I find ICD-9 codes?
ICD9Data.com takes the current ICD-9-CM and HCPCS medical billing codes and adds 5.3+ million links between them. Combine that with a Google-powered search engine, drill-down navigation system and instant coding notes and it's easier than ever to quickly find the medical coding information you need.
Are ICD-9 codes still used in 2021?
CMS will continue to maintain the ICD-9 code website with the posted files. These are the codes providers (physicians, hospitals, etc.) and suppliers must use when submitting claims to Medicare for payment.
How do I find the diagnosis code?
If you need to look up the ICD code for a particular diagnosis or confirm what an ICD code stands for, visit the Centers for Disease Control and Prevention (CDC) website to use their searchable database of the current ICD-10 codes.
Where can I find a list of ICD-10 codes?
ICD-10 CM Guidelines, may be found at the following website: https://www.cdc.gov/nchs/icd/Comprehensive-Listing-of-ICD-10-CM-Files.htm.
What is ICD-9 and icd10 codes?
Code Structure: Comparing ICD-9 to ICD-10ICD-9-CMICD-10-CMFirst character is numeric or alpha ( E or V)First character is alphaSecond, Third, Fourth and Fifth digits are numericAll letters used except UAlways at least three digitsCharacter 2 always numeric; 3 through 7 can be alpha or numeric3 more rows•Aug 24, 2015
When was ICD-9 discontinued?
On October 1, 2015, the ICD-9-CM (International Classification of Diseases, Ninth Revision, Clinical Modification) code sets used by healthcare providers in the U.S. to report medical diagnoses and inpatient procedures was replaced by ICD-10-CM (International Classification of Diseases, 10th Revision, Clinical ...
What ICD-10 codes changed in 2021?
The first new codes in ICD-10-CM 2021 are A84. 81 Powassan virus disease and A84. 89 Other tick-borne viral encephalitis. There are five more new codes under protozoal disease subcategory B60.
Why are ICD-9 codes no longer used?
Why the move from ICD-9 codes to ICD-10 codes? The transition for medical providers and all insurance plan payers is a significant one since the 18,000 ICD-9 codes are to be replaced by 140,000 ICD-10 codes. ICD-10 replaces ICD-9 and reflects advances in medicine and medical technology over the past 30 years.
What are some common ICD-10 codes?
Top 10 Outpatient Diagnoses at Hospitals by Volume, 2018RankICD-10 CodeNumber of Diagnoses1.Z12317,875,1192.I105,405,7273.Z233,219,5864.Z00003,132,4636 more rows
How do I find the ICD-10-PCS codes in a book?
1:2411:14Coding With Kate: Dissecting the ICD-10-PCS Code Book - YouTubeYouTubeStart of suggested clipEnd of suggested clipYou should look for and then it will give you the first three letters or numbers of your code whichMoreYou should look for and then it will give you the first three letters or numbers of your code which tell you which section to go into which body system it is in or chapter.
What is the difference between ICD-9 and ICD-9-CM?
The current ICD used in the United States, the ICD-9, is based on a version that was first discussed in 1975. The United States adapted the ICD-9 as the ICD-9-Clinical Modification or ICD-9-CM. The ICD-9-CM contains more than 15,000 codes for diseases and disorders. The ICD-9-CM is used by government agencies.
How to tell if you have osteochondroma?
Symptoms of an osteochondroma include: 1 A painless bump near the joints. The knee and shoulder are most often involved. 2 Pain with activity. An osteochondroma can be located under a tendon (the tough, fibrous tissue that connects muscle to bone). When it is, the tendon may move and "snap" over the bony tumor, causing pain. 3 Numbness or tingling. An osteochondroma can be located near a nerve, such as behind the knee. If the tumor puts pressure on a nerve, there may be numbness and tingling in the associated limb. 4 Changes in blood flow. A tumor that presses on a blood vessel may cause periodic changes in blood flow. This can cause loss of pulse or changes in color of the limb. Changes in blood flow resulting from an osteochondroma are rare.
What is the gene that causes osteochondroma?
Osteochondromas are thought to be associated with a gene called EXT 1. How a defect in this gene may cause the tumors is currently poorly understood. Researchers are investigating it. Because the cause of a solitary osteochondroma is unknown, doctors have not been able to find a way to prevent it.
What are the signs of a bone tumor?
Symptoms and signs of a tumor becoming cancerous are: Growth of an osteochondroma after puberty. Pain at the site of an osteochondroma.
What is it called when a tumor sticks out from the bone?
This bone outgrowth may have a stalk or stem that sticks out from the normal bone. If the tumor has a stalk, the structure is called pedunculated. If the tumor outgrowth is attached to the bone with a broader base, it is called sessile.
When does osteochondroma stop growing?
Once a child has reached skeletal maturity, the osteochondroma typically stops growing, too. In most cases of osteochondroma, no treatment is required other than regular monitoring of the tumor to identify any changes or complications.
When should a tumor be checked for cancer?
A tumor in an adult patient should be checked for cancer if it is enlarging or has become painful. Biopsy. In some cases, a biopsy may be ordered to determine if a tumor is cancerous. In a biopsy, a tissue sample of the tumor is taken and examined under a microscope.
Can a CT scan show osteochondroma?
A biopsy of the tumor tissue will confirm whether there is any cancer. When an osteochondroma becomes cancerous, it most commonly changes into a cancer called chondrosarcoma.
What are the symptoms of osteochondroma?
Most osteochondromas are asymptomatic, but 4% present with symptoms such as osseous deformity, growth abnormality, fractures or mass effect on surrounding structures . (Vanhegan, 2012) The tumors are frequently found due to cosmetic reasons, pain from friction or pressure on adjacent tissue or due to limited range of motion of the affected joint (Tarassoli, 2009; Biermann, 2002; Chin, 2000; Stieber; 2005). Pseudoaneurysm, pseudoaneurysm rupture and hemothorax associated with local osteochondroma have been reported (Vanhegan, 2012; Patel, 2015). Short stature is associated with MHE, possibly due to a local effect of osteochondromas on the active growth plates of children (Staal, 2015; Solomon, 1951).
Where is chondrosarcoma most commonly found?
Most commonly found in the metaphyses of long bones with a predilection for the distal femur and proximal tibia. The risk of malignant transformation to chondrosarcoma is approximately 1% for solitary lesions but can be up to 10% for MHE.
What is the most common benign bone tumor?
Osteochondromas are the most common benign bone tumors and are comprised of a bony prominence with a cartilaginous cap. The presence of multiple lesions is associated with Multiple Hereditary Exostosis (MHE) and the EXT genes. Most commonly found in the metaphyses of long bones with a predilection for the distal femur and proximal tibia.
Is osteochondroma a benign tumor?
Osteochondromas or cartilaginous exostoses are benign bone tumors comprised of a bony prominence with a cartilaginous cap (Geirnaerdt, 1993). Osteochondromas can occur as isolated lesions or less commonly patients have multiple lesions. The finding of multiple lesions is consistent with Multiple Hereditary Exostosis (MHE).
Is exostosis a bone lesion?
The exostosis appears as a sharply demarcated bony lesion that contains both cortical and medullary bone, continuous with the parent bone; CT or MRI may be necessary to identify this continuity (Tarassoli, 2009; Biermann, 2002; Murphey, 2000).
Is osteochondroma a developmental disorder?
Osteochondromas have been historically viewed as developmental lesions, but there is evidence supporting a neoplastic origin (Biermann, 2002; Murphey, 2000; Porter, 1999). MHE is an autosomal dominant disorder with mutations in one of three different EXT genes (Tarassoli 2009).
Where is osteochondroma seen?
An osteochondroma can be either sessile or pedunculated and is seen in the metaphyseal region typically projecting away from the epiphysis. There is often associated broadening of the metaphysis from which it arises. The cartilage cap is variable in appearance.
What is the best imaging modality to assess cartilage thickness?
MRI is the best imaging modality to assess cartilage thickness (and thus assessing for malignant transformation), the presence of edema in bone or adjacent soft tissues, and visualizing neurovascular structures in the vicinity.
Can osteochondroma be resected?
The osteochondroma can be locally resected for cosmetic or mechanical reasons. If malignant transformation occurs (~1% in solitary osteochondromas and ~5-25% with hereditary multiple exostoses) then the resultant chondrosarcoma is usually of low grade (67-85% of cases), and surgery is usually curative (70-90%) 3,5.
Is osteochondroma a benign tumor?
Osteochondromas are a relatively common imaging finding, accounting for 10-15% of all bone tumors and approximately 35% of all benign bone tumors. Although usually thought of as a benign bone tumor, they may be thought of as a developmental anomaly. They are frequently asymptomatic and have very low malignant potential if sporadic and solitary.
Do osteochondromas become more active?
During growth, osteochondromas demonstrate increased uptake on bone scans, but with time they become no more active than normal bone. Presence of increased activity in adulthood should raise the possibility of a complication (e.g. fracture, malignancy).
Is osteochondroma a chondroid?
Osteochondromas are considered a chondroid neoplasm and are primarily a part of the growth plate which separates and continues growing independently, without an associated epiphysis, usually away from the nearby joint. The medullary cavity is continuous with the parent bone, and hyaline cartilage caps them.
Other chondrogenic tumors
Cite this page: Mantilla JG, Ricciotti R. Osteochondroma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/boneosteochondroma.html. Accessed February 20th, 2022.
Osteochondroma
Cite this page: Mantilla JG, Ricciotti R. Osteochondroma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/boneosteochondroma.html. Accessed February 20th, 2022.

Popular Posts:
- 1. icd 10 code for on xarelto
- 2. icd-10 code for left shoulder tendonitis
- 3. icd 10 code for clogged milk duct
- 4. icd 10 code for pudendal neuralgia
- 5. what is the icd code for colitis
- 6. icd 9 code for chemotherapy administration
- 7. icd 10 code for left thigh abscess
- 8. icd 10 code for struck against stationary object
- 9. icd 10 code for v72.63
- 10. icd 10 code for disorder of the skin