How serious is a brain hemorrhage?
Unfortunately, research shows that elderly patients over 65 have about a 27% chance of falling in any given year. And what might be a simple bump on the head for a young person can be a severe injury in an older adult, especially those on anticoagulants or aspirin for medical issues such as deep vein thrombosis or atrial fibrillation.
Do you recognize the 12 symptoms of brain hemorrhage?
What are the symptoms of intracranial hemorrhage? Symptoms can include: Sudden, severe headache. Dizziness or fainting. Trouble with vision, speech, or movement. Confusion, extreme irritability, or sudden personality change, or coma. Fever. Stiff neck. Seizures or convulsions. Nausea and vomiting
What to know about brain hemorrhage?
What to know about brain hemorrhage
- Causes. Age is a primary risk factor for brain hemorrhage. ...
- Symptoms. A brain hemorrhage can cause a range of different symptoms. ...
- Complications. Physical therapy can be essential for recovering from some effects of a brain hemorrhage. ...
- Types. There are several types of brain hemorrhages. ...
- Diagnosis. ...
- Treatment. ...
- Prevention. ...
- Summary. ...
What ICD-10 code to use for cubchorionic hemorrhage?
Frequently Asked Questions: What is subchorionic hemorrhage ICD 10 code? Subchorionic hemorrhage ICD 10 code is O45 (15). ... Can you experience subchorionic hemorrhage without bleeding? Yes. ... What are the other causes of bleeding during pregnancy?
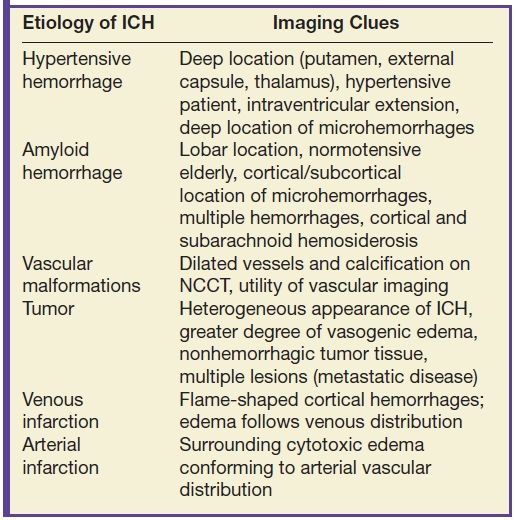
What is the medical term for cerebral hemorrhage?
Intracerebral hemorrhage (ICH) is caused by bleeding within the brain tissue itself — a life-threatening type of stroke. A stroke occurs when the brain is deprived of oxygen and blood supply. ICH is most commonly caused by hypertension, arteriovenous malformations, or head trauma.
What are 4 types of intracranial hemorrhage?
Intracranial hemorrhage encompasses four broad types of hemorrhage: epidural hemorrhage, subdural hemorrhage, subarachnoid hemorrhage, and intraparenchymal hemorrhage. [1][2][3] Each type of hemorrhage is different concerning etiology, findings, prognosis, and outcome.
What is the difference between intracerebral hemorrhage and intracranial hemorrhage?
It is important to understand the difference between the terms intracranial hemorrhage and intracerebral hemorrhage. The former refers to all bleeding occurring within the skull, while the latter indicates bleeding within the brain parenchyma. All intracranial hemorrhages (ICH) share some classic clinical features.
What is I10 diagnosis?
ICD-Code I10 is a billable ICD-10 code used for healthcare diagnosis reimbursement of Essential (Primary) Hypertension.
What is the most common intracranial hemorrhage?
Intracerebral hemorrhage: This involves bleeding inside the brain, and it is the most common type of intracranial hemorrhage and is not usually the result of an injury.
What is the difference between a brain hemorrhage and a stroke?
Although cerebral hemorrhage (bleeding anywhere inside the brain tissue itself) and hemorrhagic stroke (specifically, when a blood vessel breaks and bleeds into the brain) are most commonly associated with older adults, they can also occur in children (pediatric stroke).
Is intracranial hemorrhage the same as subdural hematoma?
This space is called the subdural space because it is below the dura. Bleeding into this space is called a subdural hemorrhage. Other names for subdural hematoma are subdural hemorrhage or intracranial hematoma. More broadly, it is also a type of traumatic brain injury (TBI).
Is a cerebral hemorrhage a stroke?
A brain hemorrhage is a type of stroke. It's caused by an artery in the brain bursting and causing localized bleeding in the surrounding tissues. This bleeding kills brain cells. Brain hemorrhages are also called cerebral hemorrhages, intracranial hemorrhages, or intracerebral hemorrhages.
Is intracerebral the same as Intraparenchymal?
Intraparenchymal hemorrhage (IPH) is one form of intracerebral bleeding in which there is bleeding within brain parenchyma. The other form is intraventricular hemorrhage (IVH). Intraparenchymal hemorrhage accounts for approximately 8-13% of all strokes and results from a wide spectrum of disorders.
Can I10 be a primary DX?
I10 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2022 edition of ICD-10-CM I10 became effective on October 1, 2021.
What is the ICD-10 code for CVA?
ICD-10 | Cerebral infarction, unspecified (I63. 9)
Is I10 a primary diagnosis?
That code is I10, Essential (primary) hypertension. As in ICD-9, this code includes “high blood pressure” but does not include elevated blood pressure without a diagnosis of hypertension (that would be ICD-10 code R03. 0).
What causes cerebral infarction?
The causes for cerebral infarction include thrombus, embolism, or stenosis. Coding of cerebral infarction provides many challenges as the codes are specific to site and there are many different ...
How many ICD-10 codes are there for FY2021?
In this part, the ICD-10-PCS procedure codes are presented. For FY2021 ICD-10-PCS there are 78,115 total codes (FY2020 total was 77,571); 556 new codes (734 new last year in FY2020)…
What is the Z20.828 code?
Assign code Z20.828, “Contact with and (suspected) exposure to other viral communicable diseases” for all patients who are tested for COVID-19 and the results are negative, regardless of symptoms, no symptoms, exposure or not as we are in a pandemic.
What is the R40.2- scale?
The coma scale codes (R40.2-) can be used in conjunction with traumatic brain injury codes, acute cerebrovascular disease or sequelae of cerebrovascular disease codes. These codes are primarily for use by trauma registries, but they may be used in any setting where this information is collected. The coma scale may also be used to assess the status of the central nervous system for other non-trauma conditions, such as monitoring patients in the intensive care unit regardless of medical condition.
How many new CPT codes were released in January?
In January, new CPT codes were released. There were 248 new CPT codes added, 71 deleted and 75 revised. Most of the surgery section changes were in the musculoskeletal and cardiovascular subsections. These included procedures such as skin grafting, breast biopsies, deep drug delivery systems, tricuspid valve repairs, aortic grafts and repair of iliac artery.
What causes cerebral edema?
Conditions that cause cerebral edema include traumatic brain injuries, ischemic and hemorrhagic strokes, brain tumors, infection, altitude sickness, electrolyte derangements, and toxins. However, the development of cerebral edema isn’t invariable; for instance, not all brain tumors have surrounding vasogenic edema.
Can a coder code exclusively from a radiology report?
The coder is not permitted to code exclusively from a radiology report.
Can cerebral edema be woven into notes?
Have cerebral edema be woven into the notes repeatedly, not just once in a single note. They should link the treatment and monitoring with the condition (e.g., “will start on Decadron for the cerebral edema and get repeat MRI in two weeks.”). It should also be present in the discharge summary.
Is traumatic cerebral edema a MCC?
If there is any loss of consciousness, in addition to those two diagnoses, there are 337 traumatic conditions, which exclude traumatic cerebral edema as a MCC. These conditions include facial and skull fractures and other types of injuries, traumatic brain injuries and hemorrhages, suicide attempts, and traumatic compartment syndromes.
Can a patient have non-traumatic cerebral edema?
It often magnifies or complicates the clinical features of the primary underlying condition. The only Excludes 1 instructions are that a patient can’t have non- traumatic and traumatic cerebral edema concomitantly.
Is cerebral edema a valid diagnosis?
It is easier to fix it on the front end than to rework it on the basis of a clinical validation denial. Cerebral edema is a legitimate, valid, important diagnosis. Get it documented in a codable format and code it.
Popular Posts:
- 1. icd 10 code for alzheimer's with vascular dementia
- 2. icd 10 code for history external hemorrhoids
- 3. icd 10 code for cryptogenic stroke
- 4. icd 10 code for arfid
- 5. icd 10 code for mssa lumbar spine
- 6. icd 10 code for dka with hyperglycemia
- 7. icd 10 code for post angioplasty
- 8. icd 10 code for pseudotumor cerebri syndrome
- 9. 2019 icd 10 code for lumbar disc protrusion
- 10. icd 10 code for 29 weeks gestation